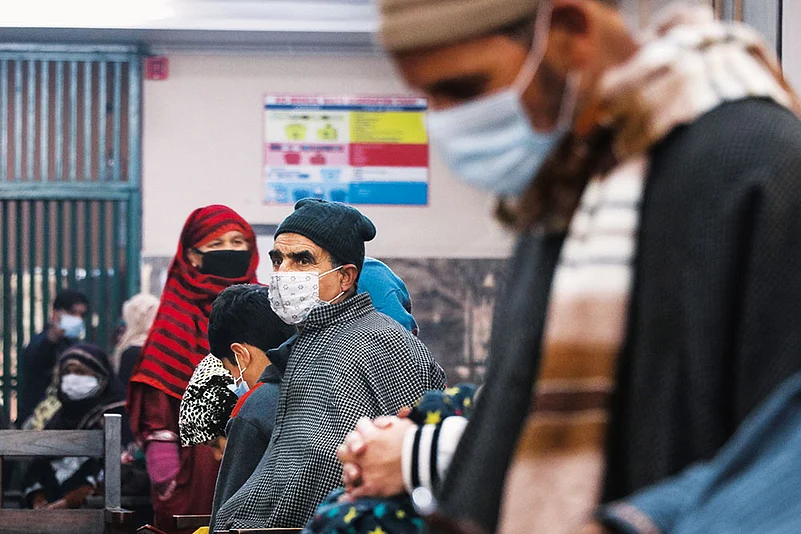
As more and more people began testing positive for COVID-19 across the country, the number of those suffering from anxiety and stress also increased. Some cases even needed urgent medical help. But with most hospitals closing down their outpatient departments (OPDs), getting correct treatment was a challenge for many.
But not for the patients visiting the Institute of Mental Health and Neurosciences (IMHANS) in Kashmir which kept its OPD doors open all through the pandemic — perhaps one of the very few medical institutions in the world to do so. In fact, to safeguard its residential patients, its doctors opposed the government’s move to convert it into a COVID hospital.
It not only admitted psychiatric patients but also patients in its de-addiction facility. “Hundreds of heroin users were admitted. They would have possibly died of drug overdose on roads had we not kept services open,” says Dr Yasir Hasan who is incharge of the addiction unit.
So, what was the need for a mental hospital to remain open in the age of online consultations? According to a community prevalence study of mental illnesses done by IMHANS in 2016, the region has a higher mental health morbidity as compared to the rest of the country due to decades of conflict. During the pandemic, the doctors witnessed a sharp increase in panic attacks and a number of COVID-19 patients developing severe psychotic symptoms when most of them had no history of any mental illness.
IMHANS knew it couldn’t neglect its patients. The institute devised its own COVID-19 safety protocols even before the government released its set of rules. These included seeing patients from a three-metre distance, always wearing masks and keeping the doors and windows of the OPD open. In case a patient was to be examined physically or a patient couldn’t wear a mask because of any reason, he or she would be directed to a ward where the doctors would be in full protective gear.
The hospital was seeing a footfall of 400-500 patients every day — almost double the normal figure before the pandemic. Soon, many seeking psychiatric treatment from different parts of the country and even from overseas began visiting IMHANS for treatment.
While it was difficult, considering the physical proximity required for the treatment of mental illnesses, it still was better than what most others were getting elsewhere. Sometimes, patients complained of confusion due to no eye contact and lack of clarity because of masks but that was the best the doctors could do. “Patients couldn’t see our smiles. They couldn’t see our facial expressions which are vital non-verbal communication in psychiatry. But they could hear us talk. There were difficulties,” says Dr Zaid, a senior doctor at the facility.
Doctors closed their private clinics for a year but came to the hospital almost every day and also ran free teleconsultation services. As per the hospital records, 2,500 telephonic consultations and 800 video consultations were done till August 2020. Telepsychiatry minimised the influx of patients to the hospital.
“I think once COVID-19 is gone, people will realise the true contribution of the hospital. Many of my colleagues and I still get messages from those whom we treated during both the waves of the pandemic,” says Dr Zaid.
The greatest achievement for the hospital, however, was that none of its in-patients contracted the virus despite 60 per cent of the hospital staff, including the HOD, getting infected with COVID-19 at various points in time. “There was no outbreak in institutional care. Had it happened in our hospital, it would have been devastating,” says Dr Wani. The hospital created its own isolation wards when there were no guidelines for it. “We devised our guidelines like in the case of schizophrenic patients,” says Dr Mohammad Maqbool Dar who narrowly survived COVID.
Now, that’s called setting an example.