Like any couple, the Singhs were elated at the birth of their baby girl, Riya. Their faces lit up at the sight of her bright eyes and playful smile, and things seemed to be going well, until, they discovered that their baby suffered from craniosynostosis – a rare syndrome often diagnosed through the absence of a soft spot on the baby’s skull. This condition occurs when the bones in a baby’s skull join together before the brain is fully formed. As the baby’s brain grows, the skull can become more malformed, causing an aesthetic problem and sometimes, a restriction to brain growth.
Needless to say, the young parents are worried – not just about the skull surgery that will be necessary, but also about the after-effects of it on their baby’s health. A surgeon will have to make a cut and separate sutures (or the fibrous joint that holds together cranial bones) leading to a lot of blood loss. The scars will take longer to heal.
It is in situations like this that Kochi-based ASIMoV Robotics, in collaboration with Dr Derick Amith Mendonca, is hoping to step in and minimise trauma. “We have been working on developing a minimally-invasive craniotomy (skull cutting) robot for the past two years,” says Jayakrishnan T, founder and CEO of the start-up. Essentially, the procedure involves making a small opening of 12-18 mm on the infant’s skull, sending a robot in to separate the sutures and getting the robot out. The working prototype is expected to be ready soon, adds Jayakrishnan.
While robots slipping into the skull are yet to be a reality, bots are being welcomed into operation theatres (OT) or are orchestrating procedures from outside it. Take what happened at Ahmedabad’s Apex Heart Institute, for instance. In 2018, a middle-aged woman had a heart attack and was diagnosed with a blocked artery. With her permission, Dr Tejas Patel, chief interventional cardiologist at the hospital, conducted the world’s first tele-robotic surgery on her. While she was lying on the hospital bed, the doctor was 32 km away in Gandhinagar and was controlling the robots performing the surgery. This procedure was executed with the help of CorPath technology from US-based Corindus Vascular Robotics.
The success of this surgery sent ripples far and wide, giving medical professionals confidence to enlist bots more often. Dr Devi Shetty, founder and chairman of Narayana Health, says, “like open surgery made way for laparoscopic surgery, laparoscopic surgery will eventually be replaced by robotic surgery”.
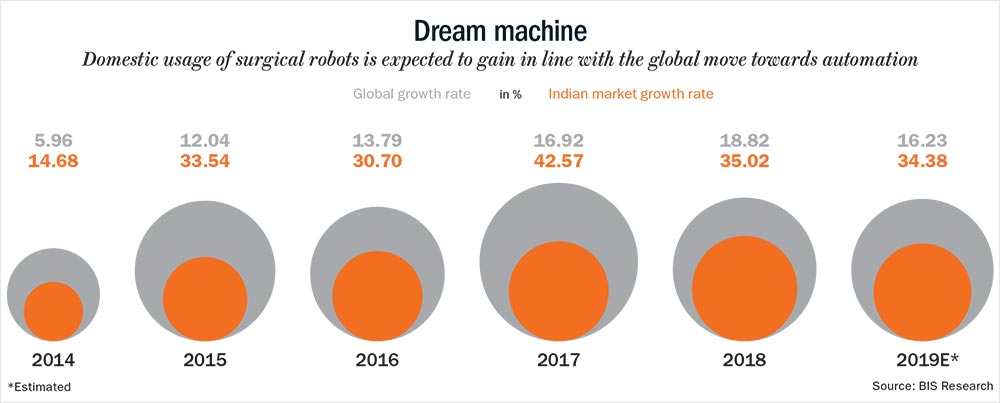
Statistics validate his observation. A report published by BIS Research, states that the global surgical robotics market is anticipated to grow to more than $12.59 billion by the end of 2025, at a CAGR of 12% during the forecast period of 2018-2025. (See: Dream machine). Closer home too, a large number of healthcare institutions — from Jaslok and Kokilaben to Fortis and Medanta — are letting bots into the OT.
Dr Ritu Garg, zonal director, Fortis Memorial Research Institute (FMRI), Gurugram says that their patients who have opted for this latest tech have given encouraging feedback and satisfaction scores. “We see huge potential in robotics. Many companies are also planning to manufacture equipment at a more affordable cost, which will give an additional thrust to its use/adoption,” adds Garg. FMRI, which installed its first robot in 2015, has completed over 250 gynae-oncological, and several urological and oncological robotic-surgery procedures.
Successful surgeries at FMRI include that of a woman with invasive bladder tumour. In majority of such cases, bladder and genital organs are removed. “Very few centres in the world are performing genital organ-sparing surgeries. But with the help of robotics, our FMRI team performed radical cystectomy and preserved her ability to bear children,” says Garg.
When earlier patients would worry about trusting their health and maybe life with cold-metallic bots, today they are better informed and take every effort to get this facility. When Surat-based Siddharth Rawal’s father Haresh was diagnosed with prostate cancer, the family had to choose between laparoscopic or robot-assisted radical prostatectomy. Siddharth says that they chose the latter because he knew “a bit” about robotic surgeries and was also advised by his local urologist to opt for it. This treatment wasn’t available in Surat, and he was hence referred to Dr TB Yuvaraja, head-robotic surgery and consultant, surgical oncology (uro-oncology), Kokilaben Hospital, Mumbai. “Dr Yuvaraja is well-known and has conducted numerous robotic surgeries and, hence, we felt confident. It has been a year since the surgery, and I am happy that my father is completely healthy, without any complications,” he says.
At Kokilaben, doctors have conducted 2,600 procedures with bots, and most were for prostate cancer and surgery of organs including kidney and uterus. Dr Yuvaraja says that these are far superior to the earlier open and laparoscopic procedures, because doctors find them easier to conduct and patients recover faster.
Shakuntala Bindal, who was detected with endometrium cancer, was dreading the months of recovery after an open or laparoscopic surgery. “I was worried because my weight is 106 kg and these surgeries require bigger incisions and lead to heavy blood loss,” she recalls. Bindal consulted Dr Rama Joshi, gynae-onco and robotic surgeon, director and HOD of gynae-oncology at FMRI and underwent a robotic surgery in April this year, and was discharged within two days. “Robotic surgery required an incision of hardly 7-8 mm… I did not even have to takebed rest after that,” she says.
There is now much excitement around surgical bots, but they are not new hands in the OT. They have been assisting in surgical procedures since the early 2000s, says Kaivaan Movdawalla, director, performance improvement practice, EY. Currently, their application is largely in urology, general surgery, gynaecology and gynae-oncology. “Within urology and gynaecology, 25-30% surgeries are robot-assisted in leading hospitals,” he adds.
Decoding the robot
So what exactly are robotic surgeries? No, a robot will not be operating on a patient on its own. Instead, they will be guided by a surgeon through a sophisticated controller. But first, it is important to understand the three main types of surgical robots — semi-autonomous systems, guided systems and tele-operation systems.
While the first two systems are widely used across the world, the tele-operation system is still in its nascent stage. In the semi-autonomous system, the robot follows a ‘surgical path’ a surgeon has preset and executes the procedure based on position commands. Though the surgeon does not intervene during the surgery, he can stop the action any time for safety reasons. Orthopaedics was among the first specialities to use this option since bones are less prone to deformation. Similarly, in neurology, this procedure can be used since the skull provides a rigid frame of reference.
In the second type, robots are used as guided systems for high levels of accuracy, such as in microsurgery, reconstruction, ophthalmology and urology. Here, the surgeon controls the robotic arm. In a tele-operated surgical robot, the surgeon gives position commands through a console placed before him. These commands are transferred to the surgical robot arms through a controller. The doctor can guide the procedure from kilometres away, like Dr Patel did from Gandhinagar.
Quick trivia here. In the mid-1980s, NASA developed tele-presence surgery to help a remotely located surgeon attend to an astronaut. This technology was further developed by the US Army in 1990s to decrease wartime mortality by bringing a surgeon’s abilities to the battlefield. This technology was then blended with minimally-invasive surgery.
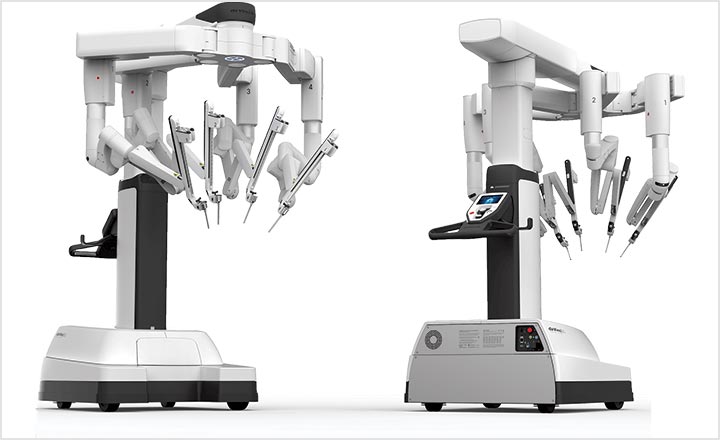
Now, who makes these robots? The company that holds a monopoly in manufacturing and supplying surgical robots is Intuitive Surgical with its da Vinci system.
It has three components — a vision cart that holds dual light source and dual three-chip cameras; a surgeon console where the surgeon sits and controls the instruments while viewing the anatomy in 3D; and a patient cart that carries the camera and instruments that the surgeon controls. The wrist, hand and finger movements of the surgeon are translated into finer manoeuvres at the tips of the instruments, which are much smaller than the surgeon’s hands, and thus work well in confined spaces.
A 2018 research paper titled The future of robotic surgery published in the Annals of the Royal College of Surgeons of England states that the da Vinci system has been the only name in invasive robotic surgery for about 20 years, mostly due to restrictive patenting, a well-developed marketing strategy and a high-quality product.
Its surgical unit sells for $0.5 million-2.5 million depending upon the model and its configuration, and the country it is being sold in. Annual revenue of da Vinci systems, led by increasing demand, has grown from $633 million in 2014 to $1.13 billion in 2018. This number constitutes 30% of the company’s total sales. In addition, they earn $700-3,500 per surgical procedure from accessories such as scalpels and forceps and an annual fee of $80,000-190,000 from after-sales service. In the first quarter of CY19, the robotic surgery player shipped 235 da Vinci systems — an increase of 27% YoY.
However, the days of it lording over the market may be coming to an end. “Today, only one manufacturer is in the market and all the surgical robots come from the US. This year, there is buzz that a few more companies may unveil their surgical robots,” says Dr Yuvaraja. The hospital did its first robotic prostatectomy for prostate cancer in May 2012.
The research paper, quoted earlier, adds that many of Intuitive Surgical’s earliest patents will be expiring in the next couple of years. As a result, the competitive landscape has been heating up with players such as Senhance Surgical Robotic System, Versius, Verb Surgical and Robodoc. Most of these are based in the US and UK, but medical institutions across the world are working to serve this industry.
An example of a new robotic system, released globally about two months ago, is the Mazor X Stealth Edition, which has been installed at the Indian Spinal Injuries Centre (ISIC) in New Delhi. The system, built by the Irish company Medtronic, is the first one to be installed in Asia-Pacific. Besides the usual advanced software jingbang, it is guided by artificial intelligence and 3D analytics. On the hardware front, its customised robotic arm can perform extremely difficult manoeuvres, particularly useful in complex procedures. Dr Harvinder Singh Chhabra, medical director and chief of spine services at ISIC, says robotic surgeries have been extremely helpful, particularly in high volume centres like theirs. “Such high improvements can drive significant clinical efficiency and reduce the burden on healthcare system in the medium to long run,” he adds.
Machine perfection
Surgeons make their career and millions with their fine motor skills. To illustrate, one slip and the knife could cut through a throbbing vein. But medical professionals cannot deny the finesse bots bring to the table.
“Robotic arms go deeper in a much finer manner, and cause less tremors while operating. In case reconstruction is required, it is done better with robotics than with laparoscopy,” says Dr Shailesh Raina, honorary director of urology at Jaslok Hospital and Research Centre, Mumbai.
Dr Raina’s views are echoed by Dr Sandeep Nayak, senior consultant-surgical oncology, laparoscopy and robotic onco-surgery, at Fortis Hospital, Bengaluru. “The greatest advantage of the technology would be 3D vision and flexible instruments available to a surgeon,” says Dr Nayak.
While surgeons benefit from having these able assistants, patients would appreciate robotic surgeries for the significantly reduced blood loss, shorter length of hospital stay (a day or two), faster recovery, and less scarring and pain, leading to lesser consumption of analgesics.
What’s more, a single robot can perform multiple types of surgeries. “It is a programmable device. All you need to do is call up the right programme and change the tools if required,” says Pradeep David, general manager, south Asia, Universal Robots. The Danish company makes smaller and more flexible collaborative industrial robot arms, known as cobots, that assist workers in improving productivity and precision. The company made its foray in India in 2016, and supplies to industries such as automotive, pharmaceuticals and FMCG at present, but sees a huge opportunity in healthcare.
Globally, countries such as Korea and the US have seen large-scale adoption of surgical robots. For instance, since 2002, Emory Saint Joseph’s Hospital, Atlanta has established a robotic surgery programme to perform heart surgery. Three years later, Korea officially began robot-assisted surgeries, when Yonsei University Health System’s Severance Hospital performed the first robotic surgery using the da Vinci system. The country has since become a popular destination for learning and undergoing robotic surgery. An article published on Analytics Insight notes that while the global robotic surgery market stood at $4.9 billion in 2016, India’s stood at $129.9 million.
Costly affair
One reason people shy away from this cutting-edge tech is the cost involved. Robotic surgery is usually #100,000-200,000 costlier than conventional procedures. Hospitals, too, have to spend a pretty penny in installing the machines. Dr Yuvaraja states that the initial investment in setting up a da Vinci robot is around #150 million-200 million.
“If we can increase the number of surgeries performed and reduce the cost, only then will we see it as a truly disruptive technology here. Otherwise, it will be limited to 5-10% of patients,” says EY’s Movdawalla. Insurance companies are only slowly catching up; Reliance Health Insurance is one of the few that covers robotic surgeries.
While cost is one barrier, another is the element of risk which cannot be wished away. “Typically, there are about 10-15% complications associated with a Robotic Assisted Laparoscopic Prostatectomy (RALP), owing to factors such as equipment malfunction, lack of surgeon training and experience. Also, if a robotic error occurs, the chances of a more sustainable injury or a permanent injury could be significant,” Movdawalla warns.
But Dr Rama Joshi of FMRI says that this would be a rare occurrence. Mechanical failures may occur, she says, but in comparison with open or laparoscopic procedures, very few surgical procedure risks have been reported with bots.
In human hands
It is a situation where benefits seem to outweigh risks, but as Dr Raina of Jaslok says, “You can use technology as a walking stick, not as a pair of crutches.” The success depends on the surgeon’s competence, not the robot’s.
So, the skill and experience of a surgeon are non-negotiable. Medical institutions need to invest in training doctors. A surgeon must learn to use the new gadget safely through training, certification and mentorship, which, unfortunately, are not sufficiently available.
Dr Joshi states that robotic surgery is a relatively new technology that requires advanced operator skill — something that is not usually learned in residency. “The facility of robotic surgeries is available in few medical schools across the country,” she adds.
A few hospitals have been proactive in building a strong ecosystem to train and to help their doctors adapt to this technology. At FMRI, for example, regular workshops and masterclasses in robotics are organised for doctors. Fortis also conducts workshops on head and neck robotic onco-surgery.
Future boom
Surgeons believe the next wave of innovation will be in automating decision-making that is typically done by a surgeon. “This will further automate many of the decisions that the surgeon typically makes before and during the surgery. Both AI and soft-tissue handling are expected to be the biggest driver of innovation in spine robotics,” adds Dr Chhabra of ISIC.
While the robots have established their competence in the OT, the scope of robotics in healthcare is much wider. For instance, Tamil Nadu-based Aurolab recently worked with cobots to manufacture intraocular lenses that help people regain vision after a cataract operation. Manufacturing of these lenses requires high-level precision, therefore Aurolab collaborated with GI India Automation and Systems, the Indian distributor of Universal Robots, to recruit a batch of cobots. The newbies fit seamlessly with the existing workforce and their integration resulted in 15% increase in product output.
In China, cobots are used in physiotherapy, acupuncture and dental procedures such as root canal. Similarly, in Copenhagen University Hospital, cobots are used to pick up, sort and load blood samples into an entry model for analysis. As a result, 90% of their sample results are ready within one hour.
The applications of robotics beyond surgery also include pharmacy dispensing systems, rehabilitation, cleaning and disinfection, and also in administrative functions such as billing.
For now, it is evident that surgical robotics is one of the fastest evolving field in science and technology. Back in 1997, Richard M Satava, professor emeritus of surgery at University of Washington, prophesied an operating room with microbots, robotic manipulators and computer-integrated surgery. We are getting closer to that vision.